Topic 11: Animal physiology (HL)
11.1 Antibody production and vaccination
Surface protein
- All organisms have unique molecules or markers on the outer surface of the plasma membrane of their cells
- These highly variable molecules are generally glycoproteins and they identify a cell as being “self” or “non-self”
- These markers are called major histocompatibility complexes (MHC)
- These MHC proteins are genetically determined and are unique to that individual
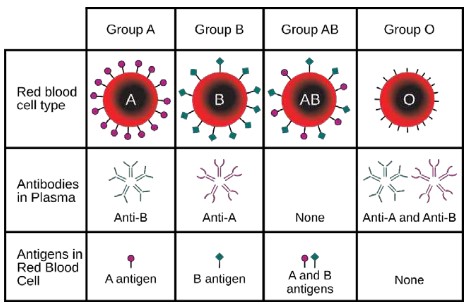
- Blood groups such as A, B, AB and O are identified by cell surface antigens
- Rhesus (Rh) is another antigen that can be present on the surface of the blood cells, being either Rh positive (has antigen) or Rh negative (doesn’t have antigen)
- A blood transfusion given to an individual with the wrong blood type can stimulate an immune response called agglutination (clumping or clotting of the blood cells)
- This is followed by the destruction of the RBC (hemolysis)
- For example, someone with blood type A (antigen A on the surface) contains anti-B antibodies in their plasma. If they get a transfusion with blood type B, their immune system will attack and destroy the foreign blood cells with the B-antigen on the surface
- People with blood type O just have the basic antigen sequence that all blood cells have and are therefore not attacked by A or B antibodies; therefore, blood type O is known as the universal donor (O negative has no Rhesus factor)
Types of pathogen
- Pathogens can be species-specific although others can cross species barriers.
- Invading organisms such as a virus or bacterium that enters the body and causes a disease are known as pathogens
- Pathogens are generally species specific, for example, humans are the only known organisms susceptible to pathogens such as polio, syphilis, measles and gonorrhea but are resistant to many pathogens that infect other organisms
- However, there are pathogens that can cross this species barrier and infect a range of hosts, such as the Rabies virus, bird flu and the Bubonic plague
- Diseases from other animals that can infect or be transmitted to humans is called Zoonosis
- The passing of diseases from different species is a growing global health concern
T lymphocytes
- When a pathogen enters the blood, the specific antigen on the surface of the membrane is identified.
- Specific phagocytes known as macrophages recognize a pathogen as a foreign entity because of the antigens on the surface.
- The macrophage engulfs and partially destroys the pathogen.
- The macrophage takes the antigens from the destroyed pathogen and displays them on the surface of the cell bound to a membrane protein called a MHC protein (called antigen presentation).
- Specific T lymphocytes receptors recognize and bind to the antigen presented by the macrophage, thus activating the T-lymphocyte.
- The activated T-cell binds to a B-lymphocyte specific to the antigen; activating the B-cell through the binding and the release of a signaling protein
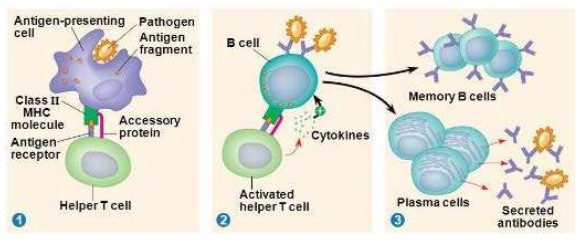
- The active B-cells begin to clone themselves producing cloned plasma B cells that produce antibodies and memory cells. Memory cells remain in the blood in case a second infection occurs to provide long term protection and a quick response to the new infection.
- The plasma cells created produce and release mass amounts of antibodies into the bloodstream.
- These antibodies surround and bind to the antigens on the foreign pathogens.
- Through a variety of different methods the pathogens are destroyed by the antibodies and other white blood cells.
Antibodies and destruction
- Agglutination – antibodies cause the sticking together of pathogens by attaching to the antigens on the surface. These clumped masses of pathogens are then easily ingested and destroyed by phagocytes
- Opsonization – antibodies make pathogens recognizable by binding to them and linking them to phagocytes, attach biological markers on pathogens
- Neutralization – Antibodies bind to toxins produced by pathogens in the blood plasma preventing them from affecting susceptible cells.
- Complement Activation – After a pathogen is identified by antibodies, complement proteins in the blood plasma form a membrane attack complex that destroys the cell membrane in the pathogen causing the cell to lyse
- Bacteria and Virus Neutralization – Antibodies can bind to the surface of viruses, preventing them from entering host cells
Immunity
- Long term specific immunity depends upon the presence of memory cells created during a previous infection from the same pathogen
- Memory cells are long-lived cells that make an effective response to a re-infection of the body by the same antigen (on the pathogen)
Vaccination
- Vaccines are introduced to the body usually through an injection but can be administered through orally or through a nasal spray
- Vaccines contain a live attenuated (weakened) or killed version of the pathogen, its toxins or one of its surface antigens.
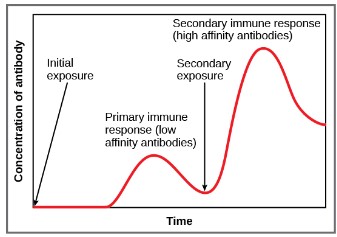
- Vaccines stimulate a primary immune response
- If the body encounters the actually pathogen, it will be destroyed right away by the antibodies during a secondary immune response
- Vaccines has made great contributions towards public health through the prevention of many deadly or dangerous diseases such as tuberculosis, measles and smallpox
Histamine
- Mast cells found in connective tissue circulating in the blood secrete histamine in response to antigens from an infection or response to an allergen
- Histamines cause the blood vessels of the infected area to dilate and increase flow of fluid containing immune components to the infected area
- It increases the permeability of capillaries so white blood cells can reach the area of infection.
- Allergies: group of condition caused by hypersensitivity of immune system to something in the environment that causes little or no problem in most people
- A number of symptoms from allergic reactions are caused by histamines
- Cells throughout the body have histamine receptors
- The release of histamine causes many of the symptoms from an allergic response such as inflammation, sneezing, itching and mucous secretion
- Anti-histamine drugs, counteract these affects by blocking histamine receptors
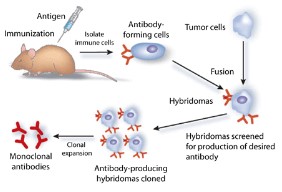
Monoclonal antibodies
- Monoclonal antibodies are identical antibodies produced by clones of a single parent immune cell that are specific to one type of antigen.
- A laboratory animal such as a mouse is injected with a specific antigen that corresponds with the needed antibodies.
- After the animal goes through a primary immune response, a plasma B-cell cell that produces the required antibody is removed from the spleen.
- Myeloma (cancer) cells are cultured in a petri dish.
- These dividing myeloma cells are mixed together with the plasma B-cells and are treated to promote a fusion between the two cells, forming a cell called a hybridoma.
- The successful hybridomas have characteristics of both cells; produce antibodies and divide rapidly for a long time.
- These hybridoma cells are cultured and allowed to divide, producing many clone cells that are able to produce large amounts of antibodies.
- Monoclonal antibodies can be extracted and used for many different applications
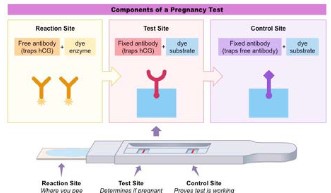
Pregnancy test
- Human chorionic gonadotrophin (HCG) is produced by an embryo in early pregnancy.
- Monoclonal antibodies can be produced by injecting a lab animal with HCG, as it recognizes this as antigen.
- HCG Antibodies are combined with color-changing enzymes.
- When the mixture is introduced into a blood sample of a woman that is pregnant, the antibodies will bind to the HCG in the blood, causing a change in color.
- If the woman is not pregnant, no HCG will be present in her blood, and therefore there will be no color change.