Topic: 11.1
The malarial pathogen, Plasmodium falciparum, enters red blood cells after a person becomes infected. After some time, each cell of P. falciparum divides to form daughter cells.
Fig. 1.1 shows a cell of P. falciparum that is forming many daughter cells.
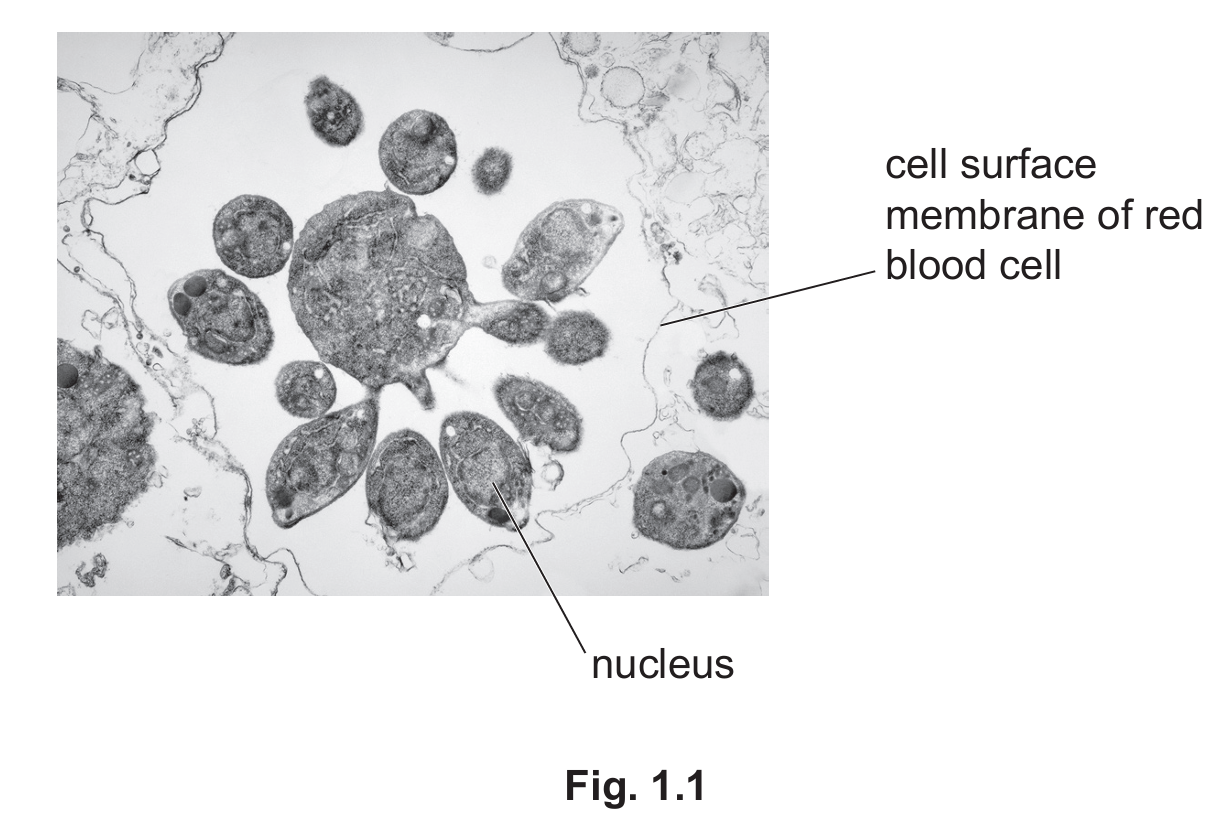
(a) With reference to Fig. 1.1, suggest how the presence of P. falciparum affects a red blood cell.
(b) When P. falciparum divides there is unequal division of the cytoplasm to form small, genetically identical daughter cells.
Outline the events that occur in the cell of P. falciparum to form the daughter cells shown in Fig. 1.1.
In 2013, the World Health Organization (WHO) set a target for researchers to create a vaccine for malaria. WHO required the vaccine to show 75% efficacy and be ready for use by 2030.
Efficacy is a measure of the effectiveness of a vaccine in reducing the number of new cases of malaria.
A trial of the R21/Matrix-M™ vaccine in Burkina Faso in 2020 achieved a 77% efficacy over a 12-month period. A control group received a vaccine for rabies.
Vaccines stimulate an immune response with the production of antibodies.
(c) Explain how antibodies will reduce the spread of the malarial pathogen through the bloodstream.
(d) Some vaccination programmes have been more successful than others.
Discuss the factors that contribute to the success of a vaccination programme.
▶️ Answer/Explanation
(a)
The presence of P. falciparum affects red blood cells in several ways:
- The red blood cell loses its normal biconcave shape and becomes irregular as the parasite grows inside it.
- The cell membrane may eventually burst (lysis) due to the pressure from multiple daughter cells forming inside.
- The parasite consumes hemoglobin and other cell contents, reducing the red blood cell’s ability to transport oxygen.
- The cell becomes filled with parasite daughter cells, compromising its normal function.
- The lifespan of the infected red blood cell is shortened as the parasite completes its life cycle.
(b)
The formation of daughter cells in P. falciparum involves several key steps:
- The parasite first grows inside the red blood cell, increasing its cytoplasm and synthesizing necessary biomolecules.
- The nucleus undergoes multiple rounds of DNA replication through mitosis, creating many nuclei.
- The cytoplasm then divides unequally around each nucleus through a process called budding.
- This results in many small daughter cells that are genetically identical but contain varying amounts of cytoplasm.
- The daughter cells remain temporarily within the original red blood cell membrane until they are ready to be released.
(c)
Antibodies combat malaria through several mechanisms:
- Antibodies bind specifically to antigens on the surface of P. falciparum, marking them for destruction.
- This binding can prevent the parasite from entering new red blood cells, blocking the infection cycle.
- Antibodies facilitate phagocytosis by white blood cells that recognize the antibody-coated parasites.
- Some antibodies can directly neutralize the parasite by blocking essential surface proteins.
- Antibodies may also cause agglutination (clumping) of parasites, making them easier targets for immune cells.
(d)
Successful vaccination programmes depend on multiple factors:
- Vaccine efficacy: Higher efficacy (like the 77% achieved by R21/Matrix-M™) leads to better disease control.
- Herd immunity: Vaccinating enough of the population to protect those who can’t be vaccinated.
- Accessibility: Making vaccines available to all at-risk populations, including remote areas.
- Public education: Combating misinformation and explaining vaccine benefits increases uptake.
- Logistics: Proper storage (especially for temperature-sensitive vaccines) and distribution systems.
- Duration of protection: Vaccines providing long-term immunity require fewer booster shots.
- Cost: Affordable vaccines that health systems can sustainably provide to entire populations.
- Strain coverage: Effectiveness against multiple strains of the pathogen prevents breakthrough cases.
- Safety profile: Minimal side effects increase public acceptance and compliance.
The R21/Matrix-M™ vaccine’s success in trials suggests it meets several of these criteria, particularly the crucial efficacy target set by WHO.
Topic: 2.2
Glucose is used in the synthesis of amylose. Glucose is first converted to glucose 1-phosphate (G 1-P).
Starch phosphorylase is an intracellular enzyme that can catalyse the synthesis of amylose from G 1-P, which is the substrate for the reaction:
\[ \text{(glucose 1-phosphate)}n \rightarrow \text{amylose + (phosphate ions)}n \]
\( n = a \) large number
Students used a colorimeter to investigate the progress of the reaction.
The students made a reaction mixture containing 0.01 mol dm\(^{-3}\) G 1-P in a buffer solution at pH 6.0. A very small quantity of amylose was added to initiate the reaction.
A solution of starch phosphorylase was added to the reaction mixture and samples were taken at 1-minute intervals. Each sample was added to a dilute iodine solution, stirred and then poured into a cuvette. The absorbance of each solution was recorded.
The results of the investigation are shown in Fig. 2.1.
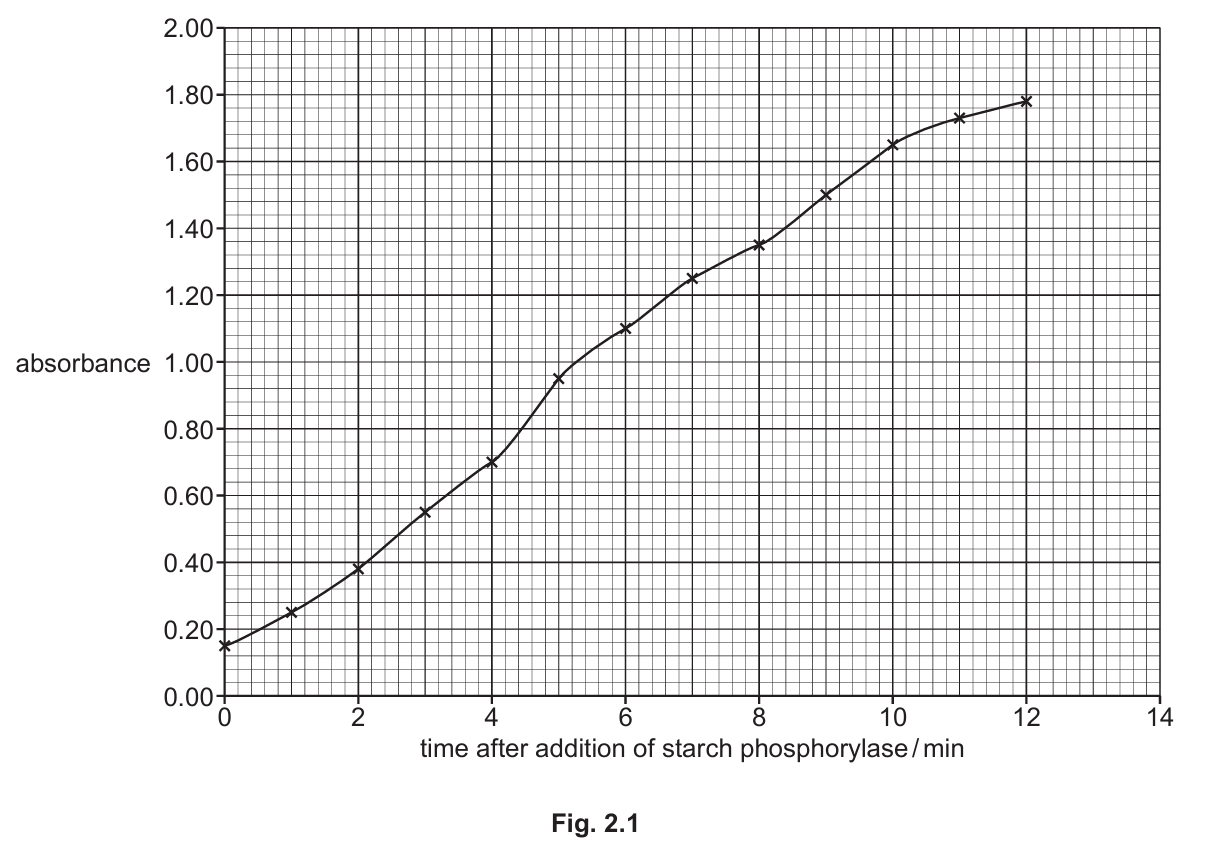
(a) (i) Explain why the absorbance increases, as shown in Fig. 2.1.
(ii) The students took their final sample at 12 minutes.
Predict the results for absorbance if the students had continued to take samples for a further 10 minutes. Explain your answer.
(iii) State an advantage of using a colorimeter in determining the progress of the reaction.
(b) The reaction catalysed by starch phosphorylase occurs at the ends of amylose molecules.
Describe the sequence of events that occurs when starch phosphorylase catalyses the addition of a molecule of glucose to the end of an amylose molecule.
▶️ Answer/Explanation
(a)(i)
More starch/amylose is produced so iodine solution becomes darker/changes from yellow-brown to blue-black.
Explanation: The colorimeter measures absorbance, which increases as more amylose is formed. Iodine forms a blue-black complex with amylose, so as the reaction progresses and more amylose is produced, the color intensity increases, leading to higher absorbance readings.
(a)(ii)
Prediction: Absorbance remains constant/reaches plateau at about 1.80.
Explanation: All the substrate (G 1-P) would be used up/converted to amylose by this point. Once the substrate is exhausted, no more amylose can be produced, so the absorbance would stabilize at its maximum value. Alternatively, the colorimeter might reach its detection limit at about 2.00 absorbance units.
(a)(iii)
Colorimeter gives quantitative/numerical results that are not subjective.
Explanation: Unlike visual assessment which can vary between observers, the colorimeter provides objective, numerical measurements of absorbance. This allows for more precise tracking of the reaction progress and enables the creation of accurate graphs and calculations of reaction rates.
(b)
1. Substrate (G 1-P) binds to the active site of starch phosphorylase, forming an enzyme-substrate complex.
2. The end of an existing amylose molecule also binds to the active site.
3. The active site changes shape (induced fit) to accommodate both substrates.
4. The enzyme lowers the activation energy for the reaction.
5. A glycosidic (α-1,4) bond forms between the glucose molecules in a condensation reaction (water is released).
6. The phosphate ion leaves the active site.
7. The extended amylose molecule is released.
Explanation: Starch phosphorylase catalyzes the addition of glucose units to the non-reducing end of amylose molecules. The enzyme brings the glucose 1-phosphate substrate and the growing amylose chain together in its active site, facilitating the formation of glycosidic bonds through a condensation reaction. This process repeats to build the amylose polymer.
Topic: 8.1
Haemoglobin is a complex protein molecule made of four separate subunits, as shown in Fig. 3.1.
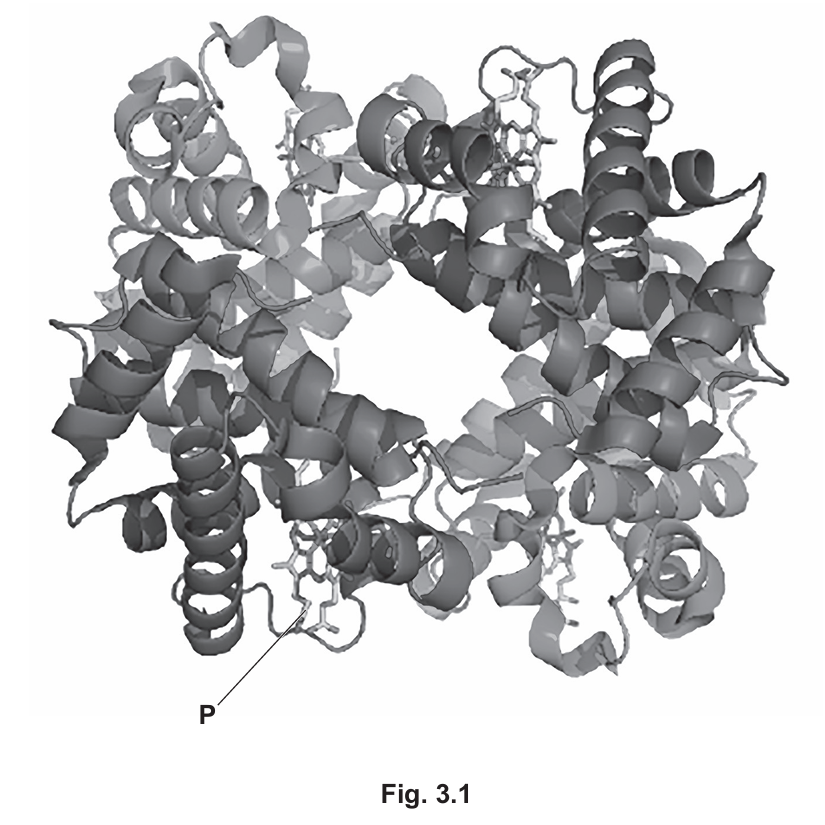
(a) (i) The shading represents the two different polypeptides that form a molecule of haemoglobin. State the names of the two different polypeptides.
(ii) Identify the structure labelled P in Fig. 3.1.
(iii) Fig. 3.1 shows some of the levels of protein structure. State the level of protein structure that is not shown in Fig. 3.1.
(b) Haemoglobin is involved in the transport of carbon dioxide. Molecules of carbon dioxide enter red blood cells as the cells travel in capillaries through muscle tissue. Some of these molecules are converted to carbonic acid. Explain how haemoglobin is involved in the transport of carbon dioxide molecules that are not converted to carbonic acid.
(c) When haemoglobin associates (binds) with oxygen it forms oxyhaemoglobin. State the precise site in the mammalian body where haemoglobin molecules bind with oxygen.
(d) The compound 2,3-diphosphoglycerate (2,3-DPG) is produced in red blood cells. 2,3-DPG binds to haemoglobin and stabilises it. Fig. 3.2 shows oxygen dissociation curves when red blood cells have high and low concentrations of 2,3-DPG.
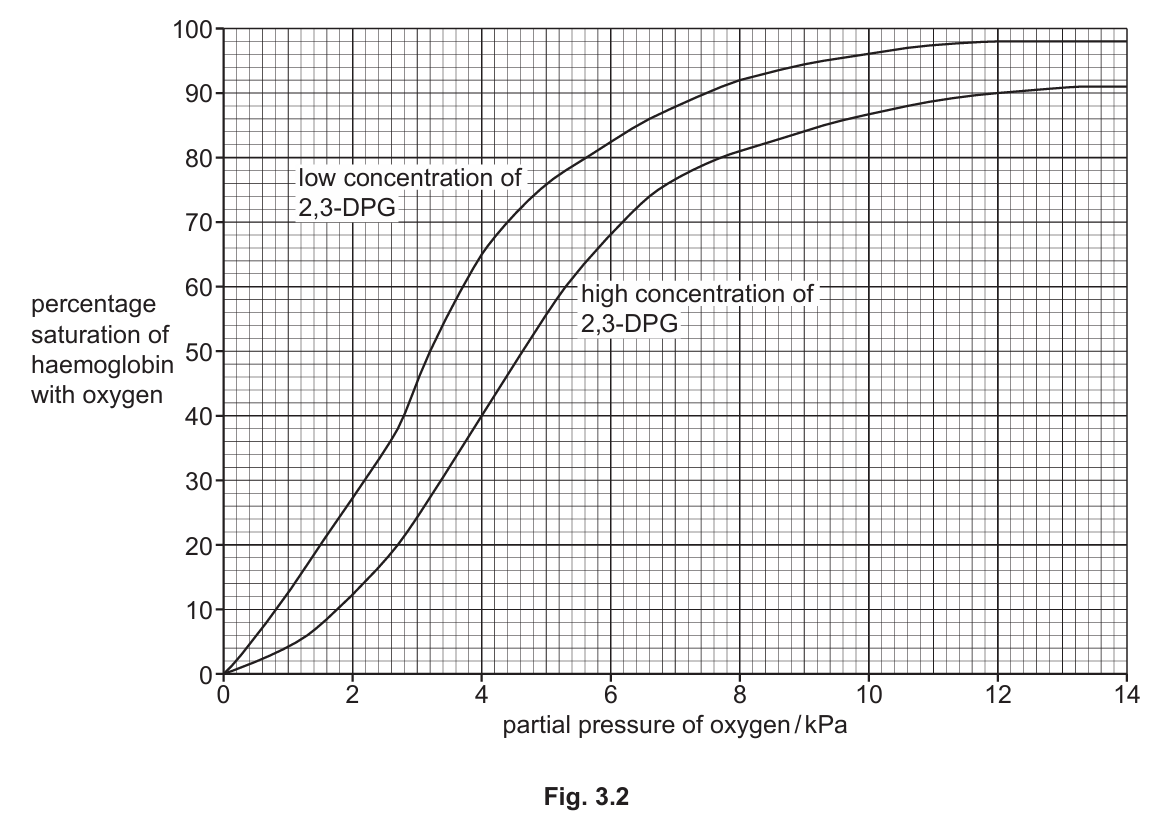
(i) Use the information in Fig. 3.2 to describe the effect of an increase in the concentration of 2,3-DPG on the oxygen dissociation curve.
(ii) Blood is stored in blood banks for use in hospitals during operations. The concentration of 2,3-DPG in red blood cells decreases when blood is stored in a blood bank. State and explain the effect that the use of blood taken from a blood bank has on the supply of oxygen to the tissues of a person during an operation.
▶️ Answer/Explanation
(a)(i) Alpha (α) globin and beta (β) globin polypeptides.
Explanation: Haemoglobin is a tetrameric protein composed of two alpha (α) chains and two beta (β) chains. These polypeptide chains are slightly different in their amino acid sequence but work together to form the functional haemoglobin molecule.
(a)(ii) Haem group.
Explanation: The structure labelled P is the haem group, which is a prosthetic group containing an iron ion (Fe²⁺) at its center. This iron ion is responsible for binding oxygen molecules in the lungs.
(a)(iii) Primary structure.
Explanation: The figure shows the quaternary structure (four subunits together), tertiary structure (folding of individual subunits), and secondary structure (alpha helices within subunits), but doesn’t show the primary structure, which is the specific sequence of amino acids in each polypeptide chain.
(b) Haemoglobin binds directly to carbon dioxide molecules at their terminal amine groups (-NH₂) to form carbaminohaemoglobin, transporting about 20% of CO₂ in this form. The remaining CO₂ is converted to carbonic acid.
Explanation: When carbon dioxide enters red blood cells, about 70% is converted to carbonic acid by the enzyme carbonic anhydrase. However, the remaining 20-30% binds directly to haemoglobin at the terminal amine groups of its polypeptide chains, forming carbaminohaemoglobin. This provides an alternative transport mechanism for CO₂. When blood reaches the lungs, the CO₂ is released from haemoglobin and exhaled.
(c) Alveolar capillaries in the lungs.
Explanation: Haemoglobin binds with oxygen specifically in the capillaries surrounding the alveoli in the lungs. This is where oxygen diffuses from the alveolar air spaces into the blood, binding to the iron ions in the haem groups of haemoglobin to form oxyhaemoglobin.
(d)(i) An increase in 2,3-DPG concentration causes the oxygen dissociation curve to shift to the right, indicating reduced oxygen affinity of haemoglobin.
Explanation: 2,3-DPG binds to haemoglobin and stabilizes its deoxygenated form, making it harder for haemoglobin to bind oxygen. This rightward shift means that at any given partial pressure of oxygen, haemoglobin will be less saturated with oxygen. The P₅₀ (partial pressure at which haemoglobin is 50% saturated) increases from about 3.2 kPa to 4.6 kPa, showing oxygen is more readily released to tissues.
(d)(ii) Blood from blood banks has reduced 2,3-DPG levels, causing haemoglobin to have higher oxygen affinity and release less oxygen to tissues during operations.
Explanation: During storage, red blood cells metabolize less and produce less 2,3-DPG. With lower 2,3-DPG, haemoglobin’s oxygen dissociation curve shifts left, increasing its oxygen affinity. This means haemoglobin holds onto oxygen more tightly and releases less to tissues during an operation, potentially causing tissue oxygen deprivation. The effect is temporary as 2,3-DPG levels are restored within 24-72 hours after transfusion.
Topic: 4.1
Fig. 4.1 is a diagram showing the transcription of part of the COL1A2 gene that codes for a collagen polypeptide. The part of the COL1A2 gene shown is a section of exon. Structure A represents an enzyme involved in transcription.
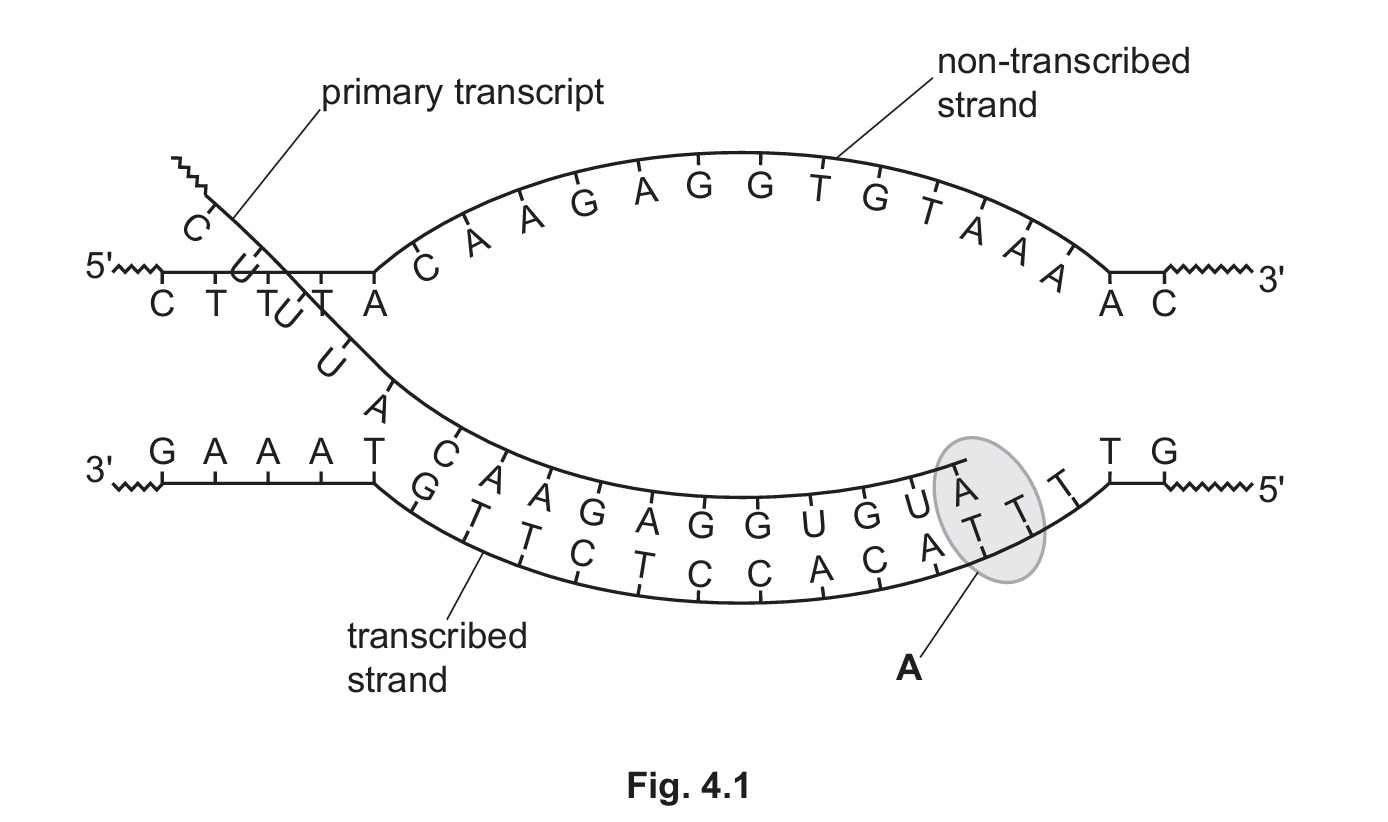
(a) (i) Name the enzyme labelled A in Fig. 4.1.
(ii) Name the bond that forms between the nucleotides in the primary transcript.
(b) (i) State the number of amino acids that are coded for by the sequence of nucleotides on the primary transcript shown in Fig. 4.1.
(ii) Use the information in Fig. 4.1 to explain why one of the strands of DNA is not transcribed.
(c) New mitochondria are formed when a mitochondrion divides into two.
Fig. 4.2 is a transmission electron micrograph of a mitochondrion that is dividing.
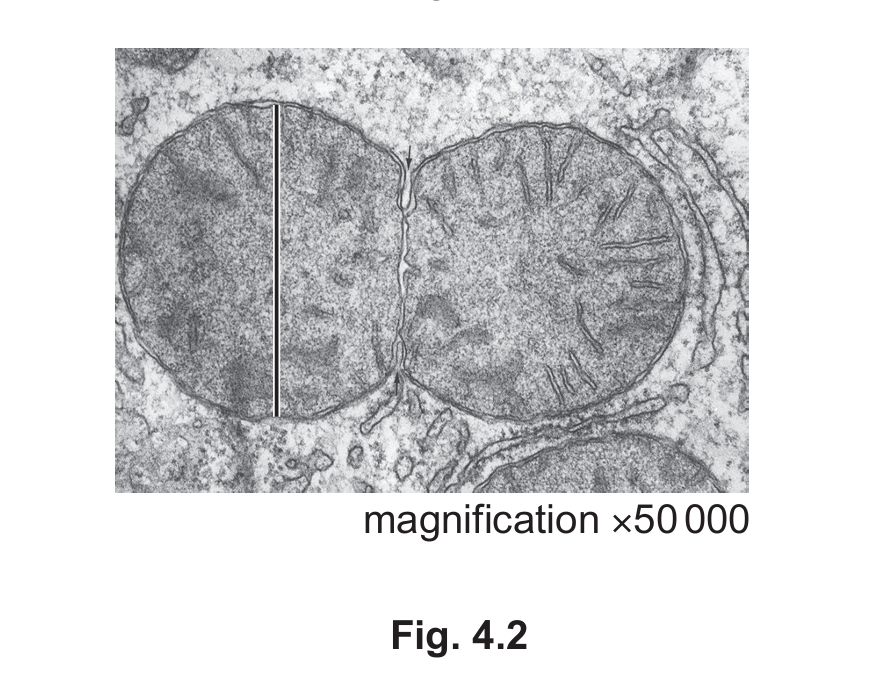
(i) State two features of mitochondria that are visible in Fig. 4.2.
(ii) The line on Fig. 4.2 shows the diameter of one of the mitochondria. Calculate the actual diameter of the mitochondrion. Give your answer to one significant figure.
(d) Mitochondrial DNA codes for some polypeptides of proteins used within the mitochondrion. Some of the proteins allow movement of ions into and out of the mitochondria. Outline the ways in which ions can move into mitochondria.
▶️ Answer/Explanation
(a)(i) RNA polymerase.
Explanation: RNA polymerase is the enzyme responsible for synthesizing RNA from a DNA template during transcription. It binds to the promoter region of DNA and unwinds the double helix to read the template strand.
(a)(ii) Phosphodiester bond.
Explanation: Phosphodiester bonds form between the phosphate group of one nucleotide and the sugar (ribose) of another nucleotide in the RNA primary transcript. These bonds create the sugar-phosphate backbone of the RNA molecule.
(b)(i) 5.
Explanation: The primary transcript shown contains 15 nucleotides (visible in Fig. 4.1). Since each amino acid is coded by a triplet of nucleotides (codon), 15 nucleotides would code for 5 amino acids (15 ÷ 3 = 5).
(b)(ii)
Explanation: Only one strand of DNA (the template strand) is transcribed because:
- The other strand (non-template strand) has a complementary sequence that would produce a different mRNA sequence if transcribed.
- Transcribing both strands would result in two different mRNA molecules coding for different proteins, which would be energetically wasteful and potentially harmful.
- The template strand is selected based on promoter sequences that RNA polymerase recognizes, ensuring only one strand is transcribed at any given gene location.
(c)(i)
1. Double membrane/mitochondrial envelope (inner and outer membranes)
2. Cristae (folds of the inner membrane)
Explanation: The TEM image clearly shows the characteristic double membrane structure of mitochondria, with the inner membrane folded into cristae to increase surface area for ATP production. Other visible features might include the matrix (inner compartment) and possibly ribosomes.
(c)(ii) 0.6 μm.
Explanation: Using the scale bar or magnification information (×50,000), we can calculate the actual size. If the measured diameter in the image is 30 mm (for example), the actual diameter would be 30 mm ÷ 50,000 = 0.0006 mm = 0.6 μm when rounded to one significant figure.
(d)
Explanation: Ions can move into mitochondria through several mechanisms:
- Active transport: Uses ATP to pump ions against their concentration gradient through specific protein pumps like the calcium uniporter.
- Facilitated diffusion: Passive movement through channel proteins (like porins in the outer membrane) or carrier proteins down their concentration gradient.
- Electrochemical gradient: Some ions like H+ move through ATP synthase driven by the proton motive force.
- Symport/antiport: Coupled transport where movement of one ion drives movement of another (e.g., phosphate enters with H+ via symport).
These transport mechanisms are crucial for mitochondrial functions like oxidative phosphorylation and calcium buffering.
Topic: 7.2
In flowering plants, transport of assimilates occurs in phloem tissue between sources and sinks.
(a) (i) Explain why a root can be a source and a sink.
(ii) State two examples of assimilates that are transported in the phloem.
(b) Describe and explain the mechanism that is responsible for the movement of phloem sap in sieve tubes.
(c) Tobacco mosaic virus (TMV) infects many crop plants. The virus passes between cells in the leaves and can travel throughout plants in the phloem.
The enzyme pectin methylesterase (PME) is involved with the production of cell walls. The enzyme is also known to influence the movement of TMV through plants. Scientists investigated the effect of PME on the transport of TMV through plants.
The scientists used three varieties of tobacco plants. Two varieties, V1 and V2, have small quantities of PME. A third variety, C, has the normal quantity of PME and was used as the control in this investigation.
The plants in each group were infected with TMV at the same time. The accumulation of the virus par5ticles transported to the leaves at the top of the plants was determined over 36 days.
The results are shown in Fig. 5.1. The arrow indicates when all the plants were infected with TMV.
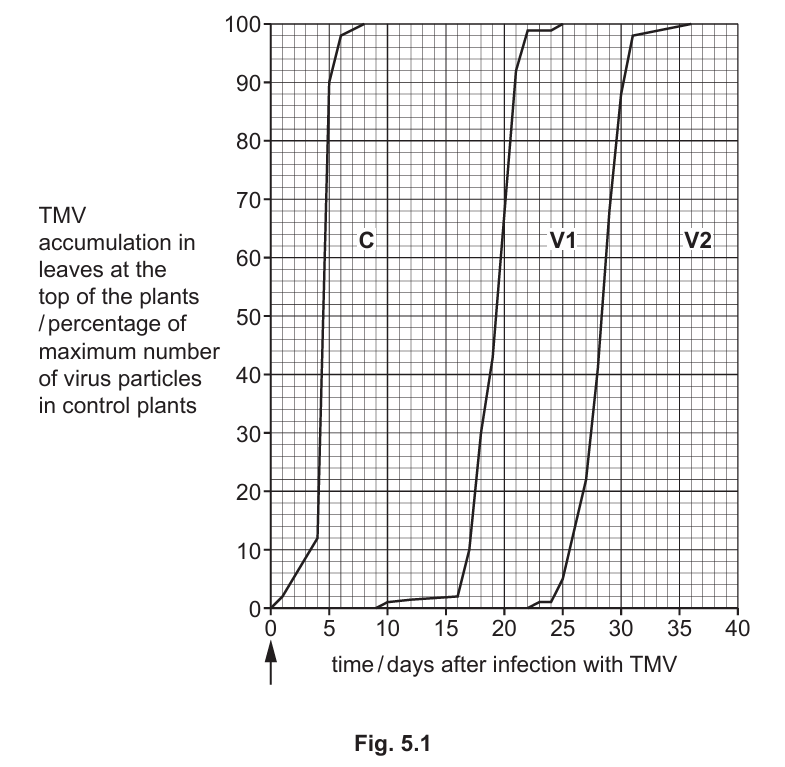
Compare the results for varieties V1 and V2 with the control group of plants, C.
▶️ Answer/Explanation
(a)(i)
Root as source: The root can provide assimilates like sucrose and amino acids for other parts of the plant when needed. This typically happens when the plant is growing and needs to distribute nutrients from storage areas.
Root as sink: The root acts as a storage organ, receiving assimilates from photosynthetic tissues (like leaves) to store for future use or to support its own growth. This bidirectional transport is a key feature of phloem tissue.
The direction of movement changes depending on the plant’s needs – during active growth periods, roots may be sinks receiving nutrients, while at other times they may serve as sources releasing stored nutrients.
(a)(ii)
Sucrose and amino acids are the main assimilates transported in the phloem. Other examples include certain hormones, mineral ions, and organic acids.
Sucrose is the primary transport sugar because it’s soluble, chemically stable, and contains high energy. Amino acids are transported as nitrogen-containing compounds needed for protein synthesis throughout the plant.
(b)
The movement of phloem sap occurs through the pressure flow hypothesis mechanism:
- At the source (typically leaves), sucrose is actively loaded into sieve tube elements from companion cells, either directly or through plasmodesmata.
- This increases the solute concentration in the phloem, lowering its water potential.
- Water then enters the phloem by osmosis from surrounding xylem vessels, creating a high hydrostatic pressure.
- At the sink (growing tissues or storage organs), sucrose is unloaded, decreasing the solute concentration.
- Water leaves the phloem by osmosis, reducing hydrostatic pressure at the sink.
- The pressure difference between source and sink causes mass flow of phloem sap through the sieve tubes.
This process is energy-dependent, requiring ATP for active loading and unloading of sugars, but the bulk flow itself is passive, driven by pressure gradients.
(c)
Comparison of TMV accumulation in V1, V2 versus control (C):
- The control plants (C) with normal PME levels showed rapid TMV accumulation, reaching maximum levels within about 8 days after infection.
- Variety V1 (low PME) showed delayed TMV accumulation, beginning around day 9 and reaching maximum levels by day 25.
- Variety V2 (low PME) showed even greater delay, with accumulation starting around day 22 and reaching maximum only by day 36.
- The rate of accumulation was slower in both V1 and V2 compared to the control, as seen by the less steep slopes of their curves.
- All varieties eventually reached the same maximum accumulation level, showing that low PME delays but doesn’t prevent full infection.
This suggests that PME plays a role in facilitating TMV movement through plants, and reduced PME levels significantly slow the systemic spread of the virus, though they don’t provide complete resistance.
Topic: 8.1
The mammalian heart consists of four chambers.
(a) Explain why the ventricles have thicker walls than the atria.
(b) Complete Table 6.1 to identify the structure in the heart responsible for each function listed.
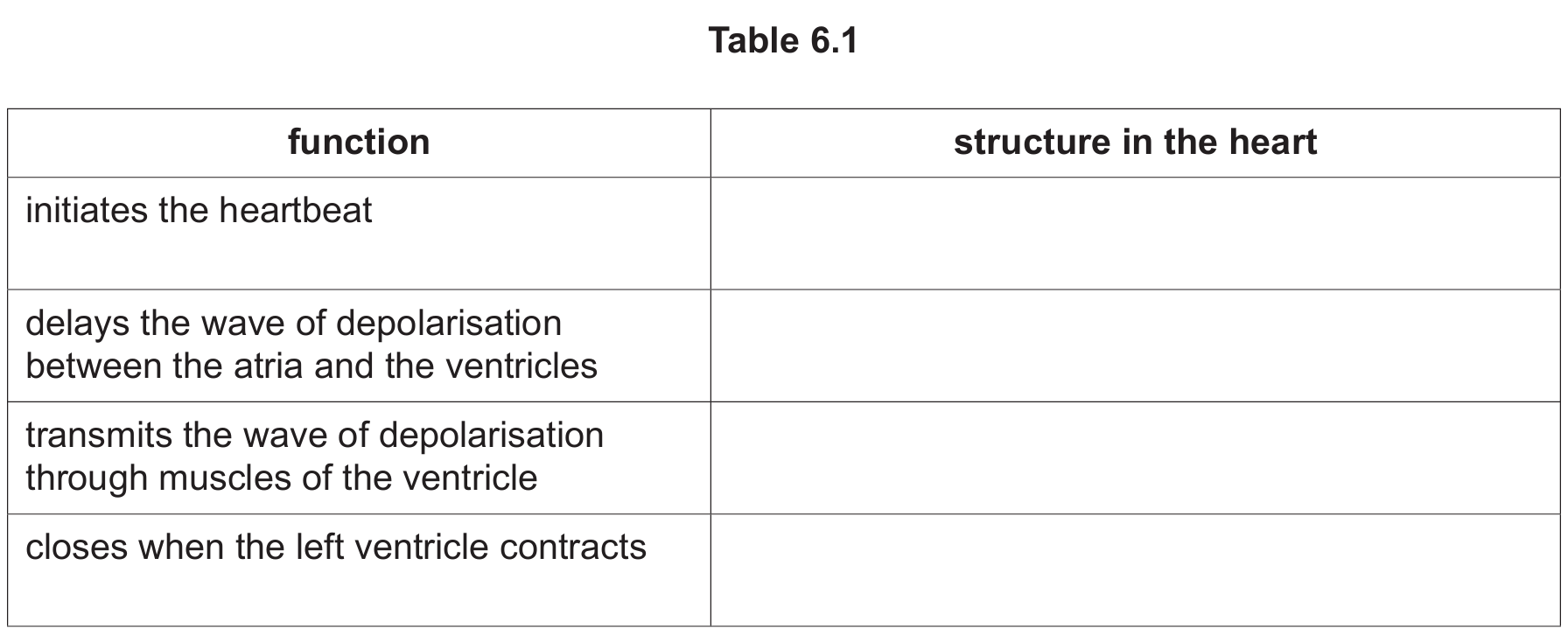
▶️ Answer/Explanation
(a)
The ventricles have thicker walls than the atria because:
- Ventricles need to pump blood over greater distances – the left ventricle pumps blood to the entire body through systemic circulation, while the right ventricle pumps blood to the lungs through pulmonary circulation.
- The thicker muscular walls allow ventricles to generate higher pressures needed for these pumping actions. The left ventricle wall is especially thick as it must overcome the high resistance of systemic circulation.
- Atria only need to pump blood the short distance to the ventricles below them, requiring less muscular force and thus thinner walls.
This structural difference reflects their different functional demands in the circulatory system.
(b)
| function | structure in the heart |
|---|---|
| initiates the heartbeat | sinoatrial node (SAN) |
| delays the wave of depolarisation between the atria and the ventricles | atrioventricular node (AVN) and non-conducting tissue |
| transmits the wave of depolarisation through muscles of the ventricle | Purkyne (Purkinje) fibres |
| closes when the left ventricle contracts | left atrioventricular (bicuspid/mitral) valve |
Explanation:
- The sinoatrial node is the natural pacemaker that initiates each heartbeat through spontaneous depolarization.
- The atrioventricular node delays the electrical impulse to ensure atria contract before ventricles, with non-conducting tissue preventing direct electrical connection.
- Purkyne fibers are specialized conducting fibers that rapidly transmit the impulse through the ventricular walls for coordinated contraction.
- The left atrioventricular valve (bicuspid/mitral valve) closes when the left ventricle contracts to prevent backflow into the left atrium.
These structures work together to ensure efficient, coordinated heart function with proper timing between chambers.
